
Discover how we can help you find relief from tarsal coalition.
Tarsal coalition occurs when two tarsal bones in the rear of the foot and the heel develop an abnormal connection by growing into each other. The tarsal coalition is composed of a bridge made of cartilage, bone or fibrous tissue. These bridges, known as bars, cover either a small area of joint space between bones or a large area. Seven tarsal bones are in the foot, including the talus, navicular, cuboid, cuneiforms and calcaneus bones, which work together to enable the motion necessary for normal foot function. Typically, tarsal coalitions form between the calcaneus bone and either the talus bone or the navicular bones.
- An estimated one in 100 people have a tarsal coalition, and about half of the cases occur in both feet.
- Many cases are never diagnosed because those with it never have noticeable symptoms.
Tarsal Coalition Symptoms
While many people are born with the condition, symptoms of tarsal coalition tend to appear between the ages of nine and 16 years. From birth until about age nine, the feet have much softer, growing cartilage. As a person ages, the cartilage mineralizes, which results in harder bones. When tarsal coalition is present, it may also harden and fuse the bones together. Sometimes there are no symptoms at the younger ages, but symptoms may appear later in life. Symptoms include the following.
- Mild to severe pain when standing or walking or with increased levels of activity
- Tired and fatigued legs
- Rigid, flatfoot in either one or both feet
- Ankle and foot stiffness, which is usually below the ankle and around the middle or back part of the foot
- Walking with a limp
- Muscle spasms in the leg that cause the foot to twist outward while walking
- Because of twisted feet and unsteady motion, ankle sprains are common and recurrent
Sometimes an ankle sprain that does not appear to improve is the first sign of tarsal coalition. Another sign could be the foot arch collapsing and reduced movement near the ankle joint.
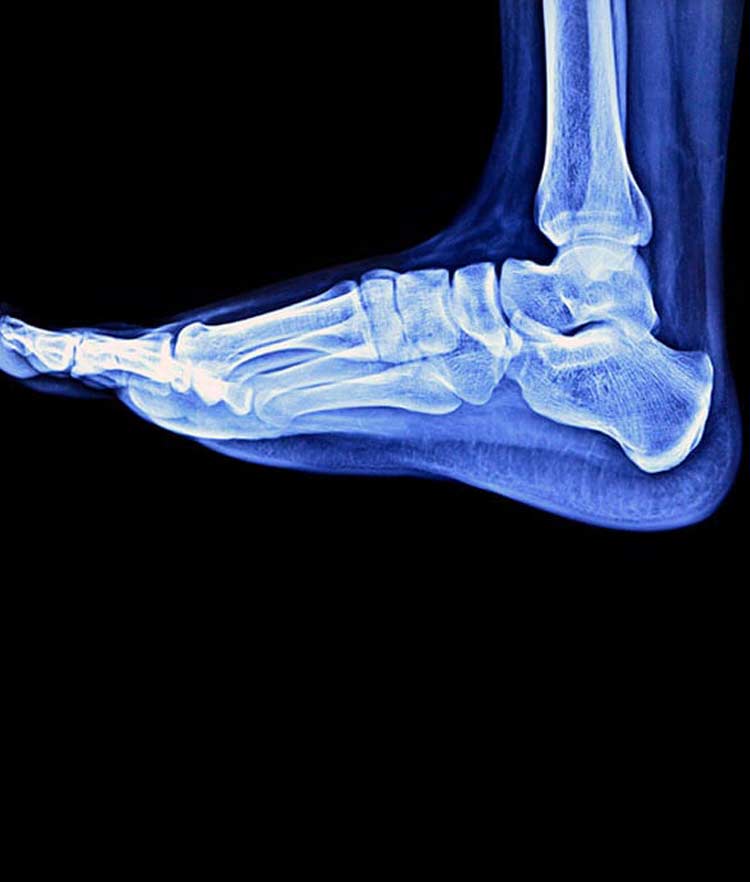
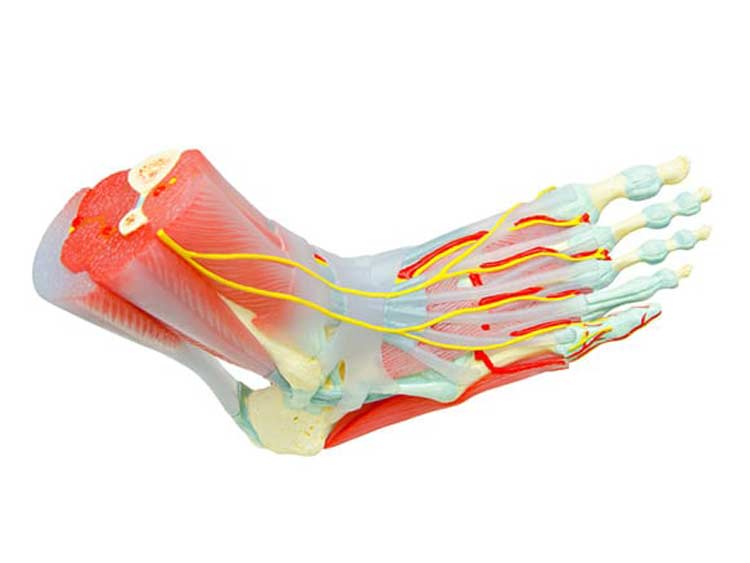
Causes
Most tarsal coalition cases begin during fetal development and are caused by mutations in the NOG gene. This gene gives instructions for producing the noggin protein, which plays a vital role in the proper development of bones and joints. Noggin binds bone morphogenetic proteins (BMPs) to keep them from triggering signals for bone development. When noggin protein does not function properly, BMPs stimulate abnormal bone formation that leads to tarsal coalition. Some instances of tarsal coalition occur later in life, usually the result of an ankle injury, arthritis in the joints or an infection.
Diagnosis and Treatment
Until bones mature, tarsal coalition is hard to diagnose in children. Often, it’s discovered in adulthood. Doctor’s examinations include checking foot flexibility and gait. Podiatrists typically order imaging tests to get an accurate image of the location and extent of the problem. This includes X-rays and CT scans to view bones and MRI scans to see soft tissue and any abnormalities.
Nonsurgical treatment, which should reduce motion of the affected joints and relieve symptoms, includes massage, ultrasound therapy, range-of-motion exercises and other aspects of physical therapy. Customized orthotics help distribute weight to limit motion at the affect joint, as well as relive pain. To let the foot rest, it is immobilized with a cast, boot or crutches. Some patients get anesthetic injections to relax spasms; this is often used before immobilization. Injections of the steroid cortisone administered directly into the joint can reduce inflammation and pain. More than one injection may be needed. Oral anti-inflammatory medicine is also used.
Surgery
When nonsurgical methods fail to relieve symptoms, surgery is an option. Size and location of the tarsal coalition, as well as any signs of arthritis in the joints, helps the doctor decide which surgical procedure to recommend. One procedure, resection, is the most common type because it successfully lessens symptoms for patients with no signs of arthritis, and it preserves normal foot motion. Fusion is the surgical choice for more severe coalitions that involve arthritis and cause significant deformity. With fusion, large pins, screws or screw-and-plate devices are inserted to hold bones in the correct position, which limits movement of painful joints.
Postoperative care requires patients to immobilize the treated foot in a non-weight-bearing cast for about three weeks. After this, they will likely wear another type of non-weight bearing cast for partial immobilization for several more weeks. When not in a cast, range-of-motion exercises are performed, and there is a gradual movement toward the patient returning to full weight-bearing ability.

