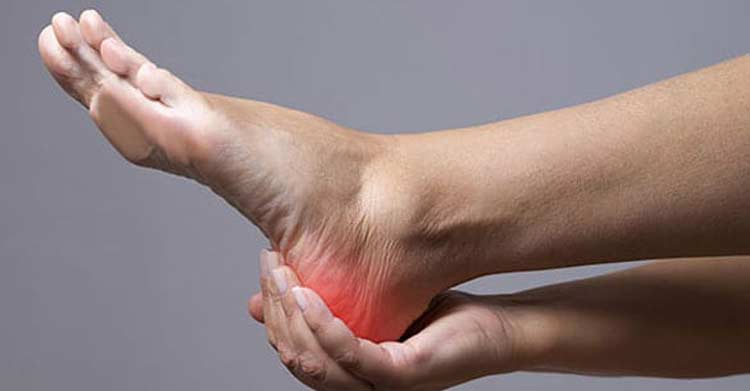
Discover how we can help you find relief from pressure ulcers.
A pressure ulcer, sometimes called a pressure sore, is a damaged area of skin that’s usually caused by remaining in one position for too long. While commonly occurring with prolonged bed rest, pressure ulcers can also develop on feet from sitting or remaining in any position that places excessive pressure on skin. If these sores are detected early, they usually go away within a few days.
- It’s when pressure ulcers go undetected or extend deeper into the skin that medical attention becomes necessary.
- If left untreated, severe pressure ulcers can lead to a serious infection.
Causes and Risk Factors
Friction on the bottom of feet is what usually causes pressure sores that eventually turn into ulcers on feet. This pressure causes skin tissues to thicken, which often contributes to calluses forming in the affected area. The thickened skin places pressure on healthy skin tissues, which causes pain. An ulcer will then form. If this added pressure isn’t relieved, a blister may form. The blister sometimes breaks and causes an open sore to develop. Health problems such as kidney disease, high blood pressure, and diabetes can increase the risk of developing pressure ulcers.
Stages
Pressure ulcers develop in stages. The first (mildest) stage is when the ulcer appears on the upper layer of skin. Symptoms at this point usually include slight discomfort or burning and itching sensations. The affected area may also be softer or firmer than surrounding skin. The second stage is when the ulcer goes deeper into the skin. It’s during this stage that a pus-filled blister may form and eventually break open. The affected area may also be swollen, red, and painful.
If a pressure ulcer reaches the third stage, it’s at a point where the related sores extend to the part of skin where fat tissues are located. At this stage, sores typically appear crater-like. There may also be a noticeable odor and drainage from the ulcer. The fourth and final stage is the most serious. This is when the sore is deeper into the skin. It could go as far as reaching ligaments, muscles, tendons, and bones. Skin often turns black at this stage as tissues become damaged enough to die. Related foot problems could make this stage even more dangerous for individuals.
Diagnosing Pressure Ulcers
If a patient is referred to a foot specialist for a pressure ulcer, it’s usually beyond the first stage. A visual inspection can determine how serious the ulcer or related sore has become. The condition of the skin in the affected area is sometimes rated on a scale that assess several factors by severity. The patient’s overall health is also considered. A blood test may also be a part of diagnosis if an infection is suspected. For deeper ulcers, an X-ray or bone scan may be done to determine the extent of the damage to tissues below the surface layer of the skin.
Non-Surgical Treatments
With mild or moderate pressure ulcers, topical creams may be prescribed to promote tissue healing. If there’s an infection, antibiotics can treat it and prevent it from spreading. It’s important for patients to take antibiotics as directed for the specified period of time. If antibiotics are discontinued too soon, the infection may return. A foot doctor may recommend custom shoe inserts or other custom orthotics to take pressure off of the affected area while the skin heals. If there is a sore, it’s usually covered with a special dressing. Patients may be instructed to keep the affected foot elevated to increase circulation and avoid placing too much pressure on the ulcer or sore.
Surgery for Pressure Ulcers
When pressure ulcers are detected while within the first two stages, non-surgical remedies are usually effective. If an infection has developed or other tissues in the foot have been affected, surgery may be necessary if antibiotics haven’t helped. Surgery may also become necessary if deeper layers of tissues are affected. The specific procedure performed will depend on the extent of the damage to tissues in the foot. Surgery often involves removal of the damaged tissue.
The National Institutes of Health (NIH) recommends placing a pillow under the base of the spine (tailbone) to prevent pressure ulcers from prolonged bed rest. On feet, they can be prevented by avoiding excessive pressure on soles, heels, or parts of the foot affected by poor circulation. Pressure ulcers can be especially problematic for individuals with existing foot conditions and underlying health issues like type 2 diabetes. If any discomfort is experienced with sores or irritations on feet, a podiatrist can determine what type of treatment is necessary and provide specific instructions for ongoing care and prevention.

