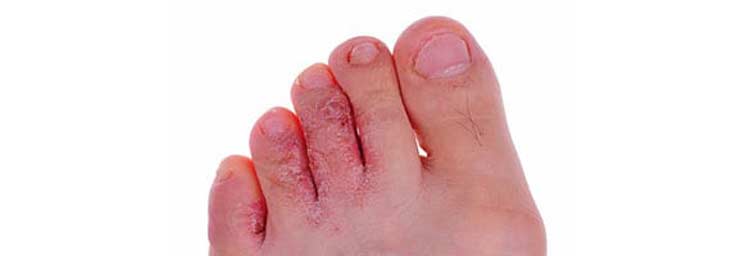
Discover how we can help you find relief from athlete’s foot.
Athlete’s foot (tinea pedis) is a fungal infection that affects skin on the foot, usually on the soles and between toes. It’s a contagious condition that can spread to other parts of the foot and sometimes other parts of the body. It’s also possible to become infected from sharing towels, socks, or shoes other individuals with this type of infection. Despite the name of the condition, anyone can get athlete’s foot.
What Causes Athlete’s Foot?
Athlete’s foot is caused by a fungal infection called trichophyton. Because this fungus thrives in warm, moist environments, it typically results in when bare feet are exposed to humid or wet surfaces, especially in common public areas like pools, locker rooms, and showers. Since such areas are often used by athletes, this is how the condition got its name. The fungal infection may also develop due to lack of proper foot care and poor foot hygiene. Additional contributing factors include:
- Sharing shoes
- Wearing the same shoes for daily use and athletic activities
- Not wearing socks with shoes
- Not washing feet after exercising, playing sports, running or jogging, or participating in other activities that may make feet sweat
Who Gets It?
It’s estimated that about 70 percent of the population will get athlete’s foot at one time or another. Anyone can be affected by this fungal infection. However, it’s more common in adolescents and adult males. It’s not usually seen in children under the age of twelve.
Common Signs and Symptoms
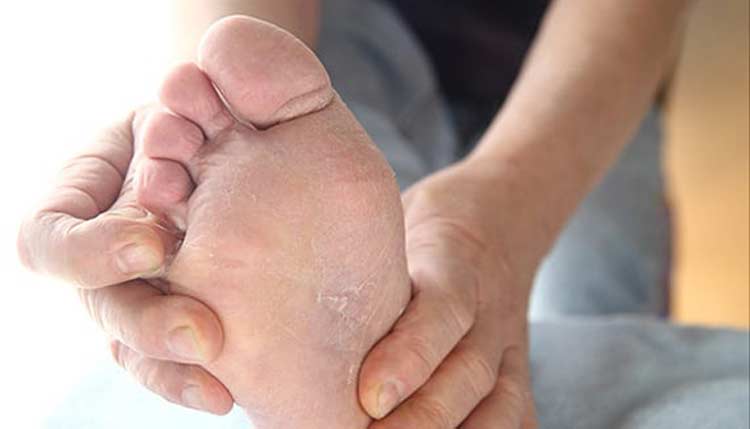
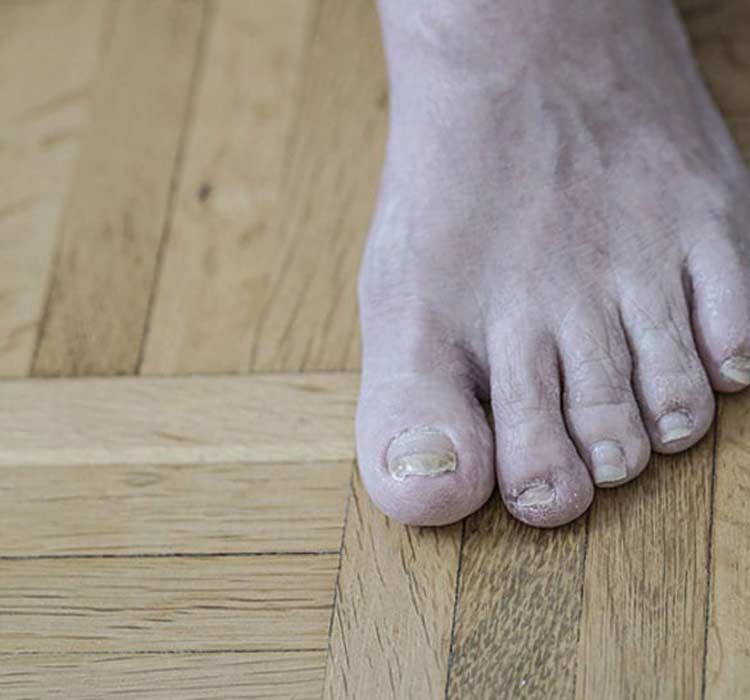
Most people notice athlete’s foot when they feel a burning or stinging sensation on the affected foot. There may also be irritation between toes or on the bottom of feet that results in the urge to scratch, although excessive scratching should be avoided to keep the infection from spreading. Scratching may also cause cuts to develop, which may make the condition more painful.
Symptoms may also include skin that’s dry, red, scaly, or flaky. Scaling patterns sometimes form on the sides or bottoms of feet. Some people with athlete’s feet may see visible swelling or blistering. If dry or red skin becomes cracked, oozing or crusting may occur. Severe athlete’s foot may cause a bacterial infection to develop on top of the fungal infection.
How Is It Diagnosed?
Athlete’s foot is usually diagnosed from a visual examination. In some instances, additional testing may be done to rule out other skin infections such as dermatitis or psoriasis. Low-grade skin infections may also produce similar symptoms.
Skin lesion potassium hydroxide is the most common test performed on patients with athlete’s foot. The potassium hydroxide that’s administered to a sample of infected tissue destroys human cells and leaves fungal ones behind. These cells are then viewed microscopically to make a diagnosis.
Treatments
Athlete’s foot isn’t serious, but it can sometimes be difficult to treat. It’s important for anyone with the condition to get in the habit of washing hands with warm soap and water to keep the fungal infection from spreading to other areas of the body. With mild cases, over-the-counter topical ointments may provide relief. If the infection persists, stronger anti-fungal medications may be prescribed. Hydrocortisone may be recommended to treat skin that’s sore or swollen. Treatment may also involve:
- Soaking feet in a solution of diluted vinegar and salt water to help blisters heal
- Tablet, powder, liquid, or spray versions of anti-fungal medications
- Oral medications like itraconazole or terbinafine for severe symptoms
What Precautions Should Diabetics Take?
Diabetics often develop athlete’s foot due, in part, to a lack of sensation in feet that can sometimes allow any discomfort from an infection to go unnoticed. The peeling and flaking often characteristic of tinea pedis can sometimes be mistaken for dry skin. If athlete’s foot goes untreated in diabetics, it may contribute to cuts and small abrasion developing.
Athlete’s foot may lead to a secondary infection that sometimes affects diabetics called cellulitis, which is a non-contagious bacterial infection. What diabetics can do is self-inspect feet daily, wear socks even when walking around home, and seek treatment for anything out of the ordinary with their feet.
Even though athlete’s foot isn’t entirely preventable since it’s a common infection, your chances of getting it can be reduced by wearing flip-flops, sandals, or shoes around pool areas and keeping feet dry. Washing feet daily, wearing breathable socks, and alternating the shoes you wear can also minimize your risk of developing athlete’s foot.

